After instrumented spine surgery, loosening of the screws or breakage of the metal rods often raises the concern, “Did fusion fail?” among patients. In this article, we discuss why fusion (bone healing) does not progress the same way in every patient, the possible causes of screw loosening and rod breakage, how these problems can be prevented, and in which situations repeat surgery may become necessary.
Why Do Screws Loosen and Metal Rods Break After Instrumented Spine Surgery?
In many spinal conditions, the frequency of instrumented (implant-based) spinal surgeries has steadily increased over the past 10 years. In the United States, it has been reported that the number of instrumented spine surgeries performed in the last decade has nearly doubled compared to the previous 10-year period.
Instrumented spine surgery is commonly performed for spinal deformities such as scoliosis and kyphosis, degenerative changes of the spine, spinal stenosis, spondylolisthesis, spinal tumors, spinal infections, and following unsuccessful non-instrumented spine surgeries.
What Is the Purpose of Instrumented (Implant-Based) Surgery?
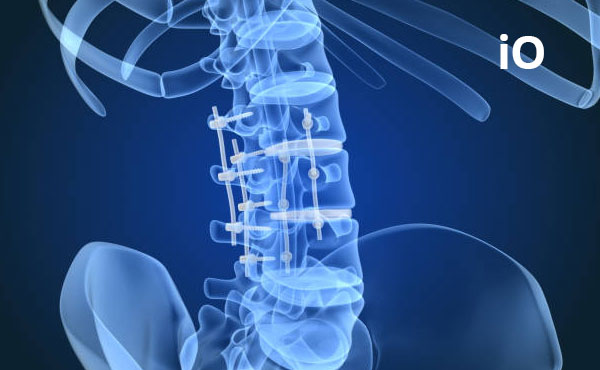
In most instrumented spine surgeries, the vertebrae are connected to each other using metal rods and screws known as pedicle screws. This limits motion between the vertebrae and aims to achieve fusion, meaning the bones heal and fuse together.
Why Do Screws Loosen and Metal Rods Break?
If fusion is not achieved—that is, if bone healing does not occur—loosening of the screws from the vertebral body or breakage of the metal rod may occur.
Rod breakage does not always mean that fusion has failed; however, in cases of screw loosening and rod breakage, the presence or absence of fusion should be carefully evaluated, particularly with computed tomography (CT).
Why Does Fusion Not Occur the Same Way in Every Patient?
The fusion process is not determined solely by the quality of the implant or the surgical procedure. Fusion is also a biological healing process. Therefore, the following factors may negatively affect this process:
- Advanced age
- Poor bone quality (advanced osteoporosis)
- Chronic diseases
- Incorrect movements or excessive strain after surgery
- Smoking
- Chemotherapy and radiotherapy in cancer patients
- Previous spinal surgeries
How Can These Problems Be Prevented?
The answer to this question can be addressed under two main headings: measures taken during surgery and management of patient-related factors.
1) Surgical techniques to enhance fusion
When instrumented spine surgery is performed using proper technique, implant failure, screw loosening, and rod breakage are quite rare, especially in growing children. The main reason is that the healing and fusion potential of the vertebrae is significantly higher in children than in adults.
In adult patients, various methods are used to improve fusion quality. One of the most commonly used approaches is the placement of cages filled with bone graft (usually harvested from the patient) after removal of the intervertebral disc between two vertebrae.
Posterior (from the back) approach
One of the most frequently used posterior techniques is transforaminal interbody fusion. In this method, during surgery performed from the back of the patient, a cage is placed adjacent to the spinal cord.
The process can be summarized as follows: first, screws are placed into the vertebrae. Then, usually under microscopic guidance, the intervertebral disc between two vertebrae is removed. If there is compression on the spinal cord or nerve roots, it is relieved, and a titanium or PEEK (polyetheretherketone) cage is placed between the vertebrae.
Anterior (from the front) approach
Another method is the anterior approach, in which the cage is placed by accessing the spine through the abdominal region. This procedure can be performed using open or minimally invasive techniques. In the anterior approach, the disc is removed from the front and cages are placed between the vertebrae.
Compared to the posterior approach, the anterior approach allows placement of larger and wider cages. This not only increases fusion rates but may also help restore lumbar lordosis and contribute to greater widening of the foramina through which nerve roots exit.
Especially in adult patients, cages placed between the vertebrae—whether via a posterior or anterior approach—can significantly reduce the risk of non-union.
2) Implant selection and surgical technique
The quality, type, and size of the screws used can influence surgical outcomes. However, the most critical factor—whether it is a primary or revision surgery—is the surgical technique itself. If the operation is not performed with proper technique, the risk of non-union remains high regardless of implant quality.
3) Optimization of patient-related factors
Patient-related factors that negatively affect fusion should be optimized as much as possible before and after surgery. Two key points stand out in this regard:
- Improving bone quality with medical treatment
- Cessation of smoking and alcohol use
Is Repeat Surgery Necessary?
When screw loosening or rod breakage is detected, a decision for repeat surgery is not automatically made in every patient. First, the severity of symptoms and their impact on daily life should be evaluated. Then, the presence or absence of fusion (bone healing) should be clarified, particularly with computed tomography.
Based on this assessment, close follow-up and medical or rehabilitation measures may be sufficient for some patients, while revision surgery may be considered for others. The decision is made by evaluating imaging findings together with the clinical picture.

